How One Accident in 1958 Revolutionized Cardiac Medicine
Three-million people worldwide all share one thing in common: their hearts beat to the rhythm of the same mistake (1). Pacemakers are used to correct irregular heartbeats known as arrhythmias, slow heartbeats, and prevent life-threatening problems (2). Traditional or transvenous pacemakers have three main components to stabilize the heart: a pulse generator, wires, and electrodes. The device delivers small electrical signals to keep the heart beating at a regular and healthy pace. The pulse generator creates the signal, the wires are embedded in the veins and carry the pulses to the heart, and the electrodes monitor the heart’s natural rhythm and send the electrical signals to correct abnormalities (3). This life-changing technology was born when electrical engineer Wilson Greatbach had initially intended to create an oscillator (4).
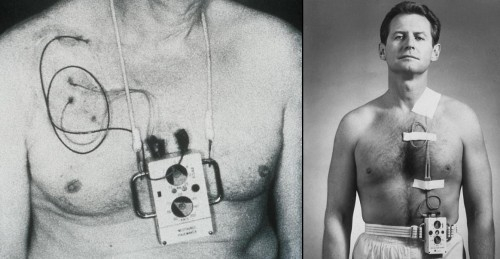
The idea of a pacemaker originated in ancient Rome (5). However, major strides toward a functional product were not made until the 1950s (5). There were many variations of Pacemakers before the implantable one used today. Paul Zoll, a Boston native, created a tabletop external pacemaker that treated heart block. Zoll’s electrodone PM-65 pacemaker monitored cardiac rhythm and had an electric pulse generator to stabilize the heart. This worked well, but was very heavy and bulky, had to be carried around on a cart, and was AC powered (5). In 1957, electrical engineer Earl Bakken developed a wearable pacemaker at the request of Dr. Walton Lillhei. It took Bakken four weeks to build a prototype, and Dr. Lillhei began to treat his patients with it almost immediately (6). The first implantable pacemaker came about only because of a strong-willed wife (5). Arne Larsson faced heart issues such as fainting episodes caused by an abnormal heart rhythm, called Stokes-Adam attacks (7). His wife, Else Marie, had heard of experimental electric stimulation and insisted her husband receive an implanted pacemaker. Her persistence led inventor Rune Elmqvist and surgeon Ake Senning to create the first implanted pacemaker. The first pacemaker Arne received failed after eight hours, but Else Marie only cared about whether he was alive. The second pacemaker lasted for a week before malfunctioning. Larsson went on to outlive both his surgeon and the engineer behind his pacemaker; he faced five lead systems and twenty-two pulse generators of eleven different models. Remarkably, his death was due to a cancer growth.
The long-term pacemaker was invented unintentionally, in 1958, when Wilson Greatbach was building an oscillator meant to record moments of increased heart rate (5) called tachycardias (8). When assembling the oscillator, Greatback intended to grab a ten kilo-ohms resistor, but when reaching into his toolbox, he accidentally pulled out a one megaohm resistor (5). The device began to set off a steady electrical pulse, and Greatbach realized the unit could be used to stabilize the human heart. Through two years of experimentation on animals, Greatbach, along with colleagues Dr. William Charduck and Dr. Andrew Gage, patented the implantable pacemaker and reported the first human success in 1960 (5). That small error in a Buffalo lab would go on to save millions of lives. Greatbach reflects in a lab journal: “I seriously doubt if anything I ever do will give me the elation I felt that day when a 2 cubic inch electronic device of my own design controlled a living heart (5).”
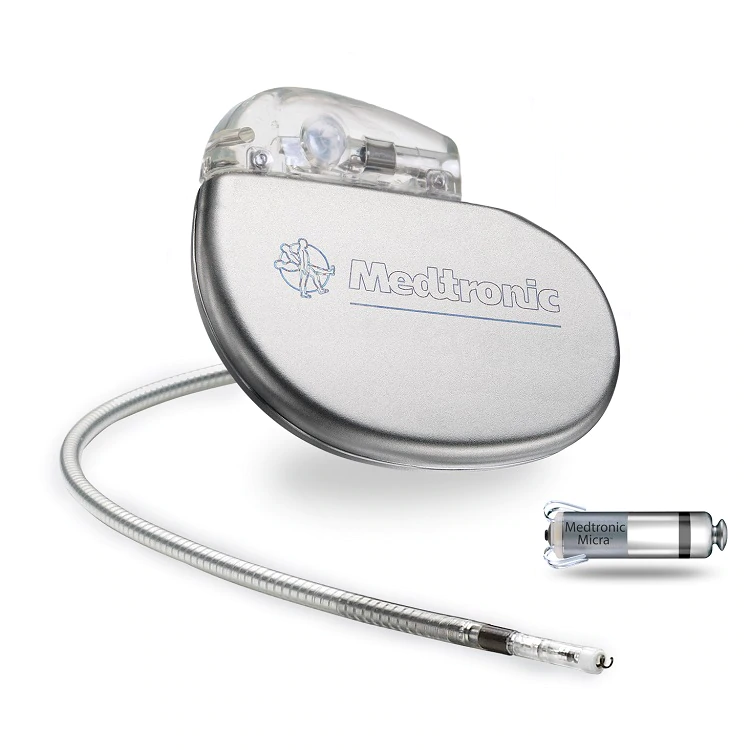
The internal pacemaker has only advanced in recent years. The traditional pacemaker invented by Charduck, Gage, and Greatbach was reliant on leads or wires to connect the unit to the heart. However, modern pacemakers have evolved to not need wires, thus lowering the risk of infection. These pacemakers are also smaller, have a longer battery life, meaning fewer replacements needed, and eliminate lead complications (10). Pacemakers used to pose a risk for MRI scans because the two devices caused an interference that turned the cardiac apparatus off (11). However, new technology has developed devices that can withstand the strong magnetic field. New pacemakers include smart technology that tracks live data, analyzes heart function, and adapts without any in-person visits (10). This allows for early detection of abnormalities or device faults and works to ensure patient safety. The traditional pacemaker needed battery replacement surgery often, but contemporary models have batteries that can last for up to fifteen years (10). Major advancements in recent times have been for comfort and functionality.
Simple mistakes can revolutionize medicine. Implantable pacemakers stemmed from a journey that started with the theorizing of Ancient Roman physicists, Zoll’s table-top bulky machine, the wearable pacemaker strapped by wires, and Else Marie Larsson, who would not take no for an answer and pushed doctors to be experimental. It took hundreds of scientists and electrical engineers who contributed their ideas, designs, and determination. But in the end, the breakthrough that would save millions of lives came down to one mistake.
Bibliography
- Cardiac Pacemaker. (2024, July 24). Yale Medicine. https://www.yalemedicine.org/conditions/cardiac-pacemaker
- Clinic, C. (2017, July 10). A pacemaker is a device implanted in your body to deliver electrical pulses to your heart. They can improve quality of life and prevent life-threatening problems. Cleveland Clinic. https://my.clevelandclinic.org/health/treatments/17360-permanent-pacemaker
- How They Work. (2022, March 24). NHLBI, NIH. https://www.nhlbi.nih.gov/health/pacemakers/how-it-works
- Wilson Greatbatch | Lemelson. (2025). Mit.edu. https://lemelson.mit.edu/resources/wilson-greatbatch
- Aquilina, O. (2026). A brief history of cardiac pacing. Images in Paediatric Cardiology, 8(2), 17. https://pmc.ncbi.nlm.nih.gov/articles/PMC3232561/
- ETHW. (2015, December 31). Milestones:First Wearable Cardiac Pacemaker, 1957-1958 – Engineering and Technology History Wiki. ETHW. https://ethw.org/Milestones:First_Wearable_Cardiac_Pacemaker,_1957-1958
- Stokes-Adams Syndrome: Symptoms, Causes & Treatment. (2023, January 26). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/24644-stokes-adams-syndrome
- Tachycardia – Symptoms and causes. (2025). Mayo Clinic; https://www.mayoclinic.org/diseases-conditions/tachycardia/symptoms-causes/syc-20355127
- Wilson Greatbatch | Lemelson. (2025). Mit.edu. https://lemelson.mit.edu/resources/wilson-greatbatch
- Ramagopal Tumuluri. (2025, February 18). How Pacemakers Are Revolutionizing Heart Care. Saak Health. https://www.saakhealth.com/how-modern-pacemakers-are-transforming-heart-health/
- Bovenschulte, H., Schlüter-Brust, K., Liebig, T., Erdmann, E., Eysel, P., & Zobel, C. (2012). MRI in Patients With Pacemakers. Deutsches Ärzteblatt International. https://doi.org/10.3238/arztebl.2012.0270
Images:






Comments are closed.