Bioethicists are coming up with point systems to decide which patients receive ventilators when in a life threatening situation.
The coronavirus pandemic has brought about many challenges with one of the most pressing ones being that there simply aren’t enough ventilators for everyone who needs one. With the number of COVID-19 cases in Massachusetts at over 56,000 as of April 28 (3), hospitals simply don’t have enough resources to provide a ventilator to every critically-ill patient. Hospitals, therefore, are struggling to come up with a generalized system for distributing ventilators in as fair of a way as possible.
Ventilators are machines that help people breathe by pushing air at the same temperature of the patient’s body into the lungs with increased oxygen (4). With COVID-19 symptoms including an assortment of respiratory conditions, they have become a treasured resource. With a predicted 2.9 million people needing ventilators according to the Johns Hopkins Center for Health Security, they are essential for most severe cases of the virus and patients can be left on them for weeks.
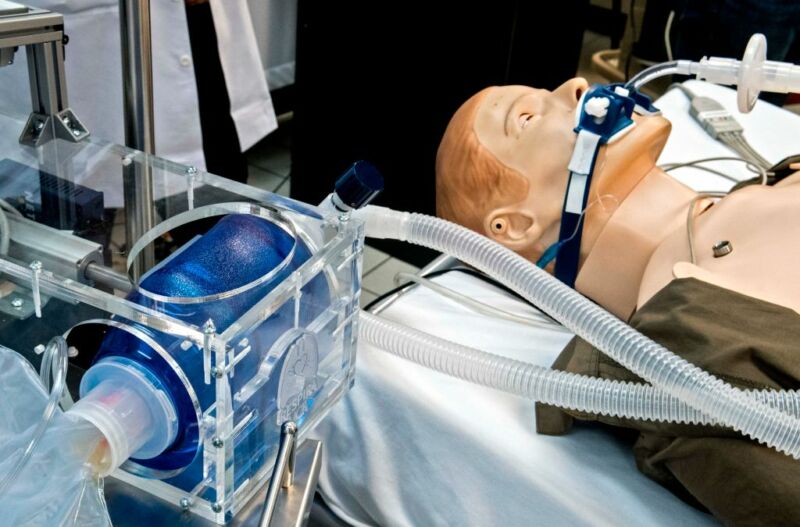
The ideal distribution of these life-saving machines has been debated by hospital officials, doctors, nurses, and bioethicists. According to bioethicist Brenden Parent, a member of the New York state task force, two different approaches have been suggested. The first approach prioritizes people who have a better chance of survival and a longer predicted lifespan. The other gives everyone an equal chance no matter their condition (2).
Dr. Douglas White from the University of Pittsburgh developed a system which Massachusetts bases its current guidelines on. It is a point system that gives each patient a score between 1 to 8 which is then used to designate access to ventilators, with patients with lower scores having increased priority. The number assigned is based on how likely it is for the patient to recover and how long they might survive after the recovery. This system, however, has its flaws as people living with disabilities or an underlying medical condition may be ranked at a lower priority (1).
Partners HealthCare, which includes Mass General and Brigham and Women’s Hospital, has developed their own strategy. They have a plan similar to the Pittsburgh system, but makes a point not to discriminate towards any group including disabilities. Furthermore, healthcare workers will not get any special treatment and will be ranked just like other patients in the system. The plan also removes ventilators from patients who seem unlikely to benefit from them: after getting put on a ventilator the patients are reevaluated once more at the 72-hour point to see if it is benefiting them.
To help with the fair distribution of the ventilators, a group of individuals, separate from the medical teams caring for patients, are making these difficult decisions. This creates a distance between the medical professionals and the decision makers. Many members of this panel are actually medical ethicists. Their job is to tally the points and share whether or not a ventilator should be offered to the patient with the medical team.
Obviously, there isn’t going to be a perfect set up that pleases everybody, but being the daughter of someone who works as a doctor at a hospital I feel a little biased about the rule that healthcare workers shouldn’t get special treatment. Doctors and nurses are getting called in to the hospital to help out in areas that they haven’t practiced in in many years. It is part of their job to help and they took an oath, but they are risking their own health and safety as per requests of the hospital, so shouldn’t they get prioritized (1)?
There currently isn’t a final plan and certain hospitals in Massachusetts such as Mass. Generals are currently working to double the amount of ventilators as more will be needed as the pandemic starts to peak (1). We are fortunate to live in a state with exceptional hospitals. Unfortunately there are only so many resources to go around. At some point, tough decisions may need to be made.
– Sofia Chen
References
- Kowalczyk, L. (2020, April 7). Who gets a ventilator? New gut-wrenching state guidelines issued on rationing equipment – The Boston Globe. Retrieved from https://www.bostonglobe.com/2020/04/07/metro/massachusetts-officials-release-plan-ration-ventilators-icu-beds-if-need-arises/?s_campaign=bdc:globewell:trending
- Ariana Eunjung Cha, L. M. G. (2020, April 7). Who gets a shot at life if hospitals run short of ventilators? Retrieved from https://www.washingtonpost.com/health/2020/04/07/ventilators-rationing-coronavirus-hospitals/(
- COVID-19 Cases, Quarantine and Monitoring. (2020, April 19). Retrieved April 19, 2020, from https://www.mass.gov/info-details/covid-19-cases-quarantine-and-monitoring
- COVID-19 Cases, Quarantine and Monitoring. (2020, April 19). Retrieved April 19, 2020, from https://www.mass.gov/info-details/covid-19-cases-quarantine-and-monitoring
Images
